This year, International Nurses Day and International Day of the Midwife may not have been celebrated as festively as many would wish; COVID-19/SARS-CoV-2 has derailed many plans and sadly led to the death of over 300,000 individuals globally, including 102 Australians at the time of report.
Unfortunately, these numbers will undoubtedly grow as the pandemic unfolds. That the developed nations of the United States, United Kingdom, and Italy account for over half of the COVID-19 fatalities worldwide, and the US by far the principal contributor to all reported deaths is one of the more disturbing facts.
While current figures appear low in comparison to deaths associated with the influenza pandemic of 1918 (approximately 50 million deaths), our ability to prevent, and treat infection has advanced considerably in the last century, an achievement that has been driven by the work of nurses and midwives.
As a novel (newly discovered) virus, COVID-19 presents several issues that fall beyond our current knowledge. While airborne transmission via small droplets has not been ruled out completely, it has also not been confirmed or fully understood (Meselson 2020). As aerosols exist on a continuum with droplets, identifying the pathogenicity of the SARS-CoV-2 virus in air samples is neither straightforward nor easily achieved independently of other potential transmission factors, particularly in real-world scenarios.
The most pressing issue however, is the lack of a vaccine. There is currently no known cure for COVID-19 and if a vaccine is developed, it will be a world-first for coronaviruses – no small feat, especially if it can be developed within the coming months. Until this time, the fundamentals of infection control and prevention are the most effective weapons in our fight against COVID-19. Interventions that nurses and midwives know well; like the backs of their (clean) hands.
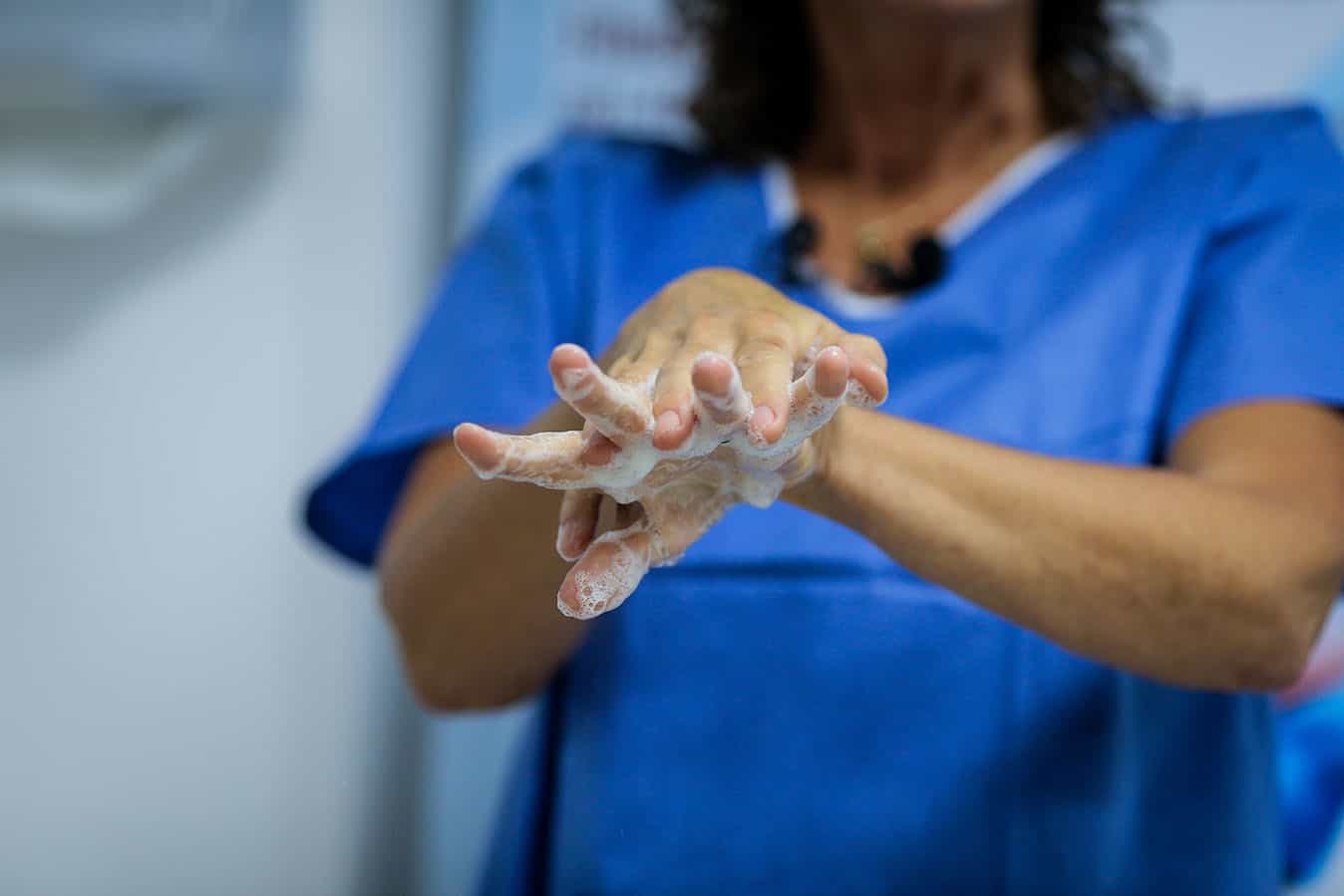
Infectious viral particles can remain on the skin (exactly how long for is unknown – but still long enough to pose a risk). Correct and frequent hand hygiene particularly hand washing (over hand sanitiser) is therefore one of the most effective barriers to infection; nurses are well-placed to ensure that colleagues, patients, and community members are aware of this (Perkins 2017).
Proper cough/sneeze etiquette, avoiding touching the face – particularly the mouth, nose, and eyes as well as other objects or surfaces which may be contaminated, and ensuring that regularly touched surfaces are properly cleaned are also effective ways of reducing infection risk.
Maintaining distance between people is one of the more controversial contemporaneous recommendations in the raft of measures advocated by governments and organisations. This may be because there are confusing differences; the World Health Organization suggests one metre (WHO 2020), the US Centers of Disease Control and Prevention suggests two metres (US CDC 2020), and the Australian government suggests one and a half metres (Department of Health, 2020). Each isn’t necessarily incorrect, but this is because none are based on solid, empirical evidence (Bourouiba, 2020).
While saliva and mucus droplets and aerosols can travel beyond two metres from an uncovered sneeze or cough (Bourouiba 2020; Tang et al. 2013), combined with cough/sneeze etiquette the recommendations encourage people to remain a reasonable, but practical distance from one another to reduce the risk of transmission particularly in poorly ventilated, indoor environments. They also limit the number of people permitted in various settings which limits contacts.
With new evidence regarding COVID-19 continually emerging and often replacing or building upon existing information and recommendations it is important that nurses and midwives strive to maintain an up to date awareness of the best available evidence and to understand that inconsistent evidence may indicate a requirement for further investigation – no easy task, given already busy schedules and large patient loads. To support nurses, midwives, and care workers, the ANMF has developed a series of Evidence Briefs to provide succinct, up-to-date, evidence on key topics regarding COVID-19, available here: anmf.org.au/campaign/entry/coronavirus-covid-19-informationfor-members
While the first (and hopefully only) wave of COVID-19 appears to be subsiding in most parts of Australia, we’re not out of the woods yet. Nurses, midwives, and carers have performed and will continue to perform excellently across their roles in health, maternity, and aged care keeping all members of the community, their patients, and clients safe. While celebrations may have been subdued this year, this year’s days for honouring nurses and midwives reminded many of the valuable role you all play on the front line of Australian and global health. Thank you.
References
Bourouiba, L. 2020. Turbulent Gas Clouds and Respiratory Pathogen Emissions Potential Implications for Reducing Transmission of COVID-19. JAMA, 323, 1837-1838.
Australian Government Department of Health. 2020. Providing health care face to face during COVID-19 [Online]. Australia: Australian Government Department of Health. Available: https://www.health.gov.au/news/health-alerts/novel-coronavirus-2019-ncov-health-alert/coronavirus-covid-19-advice-for-the-health-and-aged-care-sector/providing-health-care-face-to-face-during-covid-19 [Accessed 15 May 2020].
Meselson, M. 2020. Droplets and Aerosols in the Transmission of SARS-CoV-2. The New England journal of medicine, NEJMc2009324.
World Health Organization (WHO). 2020. Infection prevention and control during health care when COVID-19 is suspected [Online]. Geneva, Switzerland: WHO. Available: https://www.who.int/publications-detail/infection-prevention-and-control-during-health-care-when-novel-coronavirus-(ncov)-infection-is-suspected-20200125 [Accessed 15 May 2020].
Perkins, A. 2017. Hand hygiene. Nursing made Incredibly Easy, 15.
United States Centers for Disease Control and Prevention (US CDC). 2020. Interim Guidance for Public Health Personnel Evaluating Persons Under Investigation (PUIs) and Asymptomatic Close Contacts of Confirmed Cases at Their Home or Non-Home Residential Settings [Online]. US CDC Available: https://www.cdc.gov/coronavirus/2019-ncov/php/guidance-evaluating-pui.html [Accessed 28 Mar 2020].
Tang, J. W., Nicolle, A. D., Klettner, C. A., et al. 2013. Airflow dynamics of human jets: sneezing and breathing – potential sources of infectious aerosols. PLoS One, 8, e59970.
Authors
Dr Micah D J Peters, ANMF Federal National Policy Research Adviser & Casey Marnie, ANMF Federal National Policy Research Adviser Assistant.
Both are based in the Rosemary Bryant AO Research Centre, UniSA Clinical and Health Sciences, University of South Australia