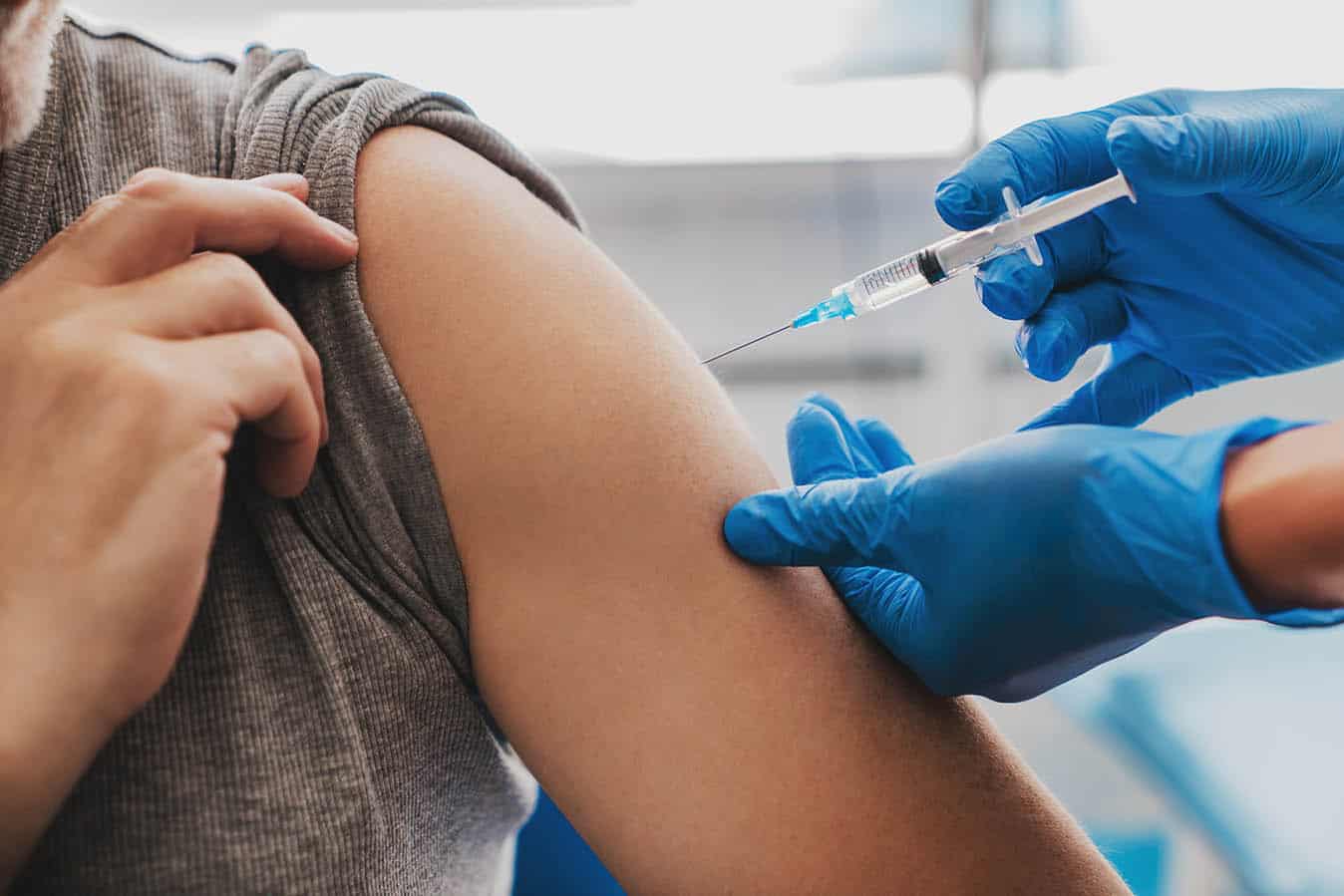
The benefits associated with COVID-19 vaccines (including Pfizer/ Comirnaty and AstraZeneca) outweigh the potential risk of adverse reactions and side effects.
Key points
- The Pfizer/Comirnaty and Oxford/AstraZeneca vaccines are safe, efficacious, and effective against SARS-CoV-2 and the SARS-CoV-2 Delta variant.
- Lack of vaccine uptake puts vulnerable members of the community at risk.
- The benefits associated with COVID-19 vaccine administration (both Pfizer/Comirnaty and Oxford/AstraZeneca) outweigh the very small but potential risks of serious adverse reactions for most people.
- Severe reactions to COVID-19 vaccines are extremely rare.
- Most reactions to COVID-19 vaccines are mild, temporary, and typical for all vaccines.
- The development of blood clots (thrombosis and thrombocytopenia/ TTS) following administration of the Oxford/AstraZeneca vaccine is extremely rare (around 2.6 cases per 100,000 among people aged under 50 and 1.6 per 100,000 among people aged 50 and older).
- It is important that all nurses, midwives, and personal care workers receive COVID-19 vaccines if they can.
Introduction
While Australia’s COVID-19 vaccine rollout has been impacted by delays, both the Pfizer/Comirnaty and Oxford/AstraZeneca vaccines are safe, effective, and efficacious for protecting people against the risk of developing severe COVID-19 infection including from the more recently identified ‘Delta’ variant.
COVID-19 vaccines in Australia
The Australian Therapeutic Goods Administration (TGA) has provisionally approved two safe, efficacious vaccines for administration in Australia; Pfizer/Comirnaty,[1] and Oxford/AstraZeneca.[2] Safety and efficacy is determined through analysis of ongoing clinical trials, international collaboration, and advice from the Advisory Committee on Vaccines (ACV). The TGA continually monitors the safety, quality, and efficacy of all vaccines before and following provisional approval.[3],[4]
AstraZeneca
Confirming earlier findings,2,[5],[6] a Phase III AstraZeneca trial with 32,449 participants found 76% efficacy for preventing symptomatic COVID-19 (Confidence Interval (CI): 68-82%) at 15 days or more after two doses given four weeks apart.[7] For adults aged 65 and older, this jumped to 85% (CI: 58 to 95%). Importantly, results showed 100% efficacy for preventing severe or critical disease and hospitalisation. No safety concerns related to the vaccine were reported.7 Another study with 156, 930 adults aged 70 years and older who reported COVID-19 symptoms found effectiveness against development of symptomatic illness of 60% (41 to 73%) from 28 to 34 days post-vaccine, increasing to 73% (27 to 90%) from day 35 onwards.[8] Also, AstraZeneca vaccination reduced the risk of emergency hospitalisation by 37% (3 to 59%) and one dose was found to be 80% effective at preventing hospital admission.
Pfizer (Comirnaty)
Confirming previous results on Pfizer/Comirnaty,[9] a Phase III trial with 46,307 participants including 927 confirmed symptomatic cases found 91.3% efficacy (CI: 89 to 93.2%) against COVID-19 from seven days to six months following the second dose. The United States Centers for Disease Control and Prevention found that the vaccine has been shown to be 100% effective (CI: 88 to 100%) in preventing severe disease. The safety and tolerability of the vaccine is high with no serious safety concerns reported from among 44,000 participants including over 12,000 participants at six months or longer following the second dose. Evidence regarding effectiveness in real world contexts suggest that the vaccine is effective for reducing risk of infection, symptomatic COVID-19, hospitalisation, and severe disease.[10],[11],[12] Receipt of the Pfizer-BioNTech or Moderna COVID-19 vaccines has been shown to be 94% effective (CI: 49 to 99%) against COVID-19 hospitalisation among fully vaccinated adults and 64% (CI: 28 to 82%) effective among partially vaccinated adults aged ≥65 years.[*][13]
Vaccines and the Delta variant
Vaccination remains a key defence to protect the community against infection, illness, and death.[14] The Delta variant appears to have greater resistance to Australian COVID-19 (Pfizer/Comirnaty and Oxford-AstraZeneca) vaccines particularly when only one dose has been administered; 33% effectiveness for protecting against symptomatic disease.[15] Two weeks after the second doses, the Pfizer/Comirnaty vaccine has been found to be 88% effective and the Oxford-AstraZeneca vaccine 60% effective for protecting against symptomatic disease which is similar to the vaccines’ effectiveness against the non-variant virus as reported.[16] A recent study from the United Kingdom reported that compared with unvaccinated individuals, following one vaccine dose, people were 75% less likely to be hospitalised, and fully vaccinated people were 94% less likely to be hospitalised.[17]
Mild vaccine reactions
Many vaccines including those for COVID-19 can cause mild reactions.[18],[19] Reactions are typically mild and disappear within a couple of days. Common reactions are; injection site pain, redness, or swelling, mild fever, and headache.5,14,[20] Less common reactions include flu-like symptoms such as muscle aches, chills/fever, nausea, or fatigue.5,14
Allergic reactions
Allergic reactions to COVID-19 vaccines are very rare. Allergic reasons can include increased redness, pain, or a rash, itching, or more extensive swelling (ie. limb swelling).[21],[22] If a person is known to be allergic to an ingredient in one of the vaccines – polyethylene glycol (PEG) in the Pfizer/Comirnaty vaccine)[23] or polysorbate, an ingredient in the AstraZeneca vaccine,[24] they should not receive that vaccine. Unless a person has experienced an allergic reaction to the first dose of a COVID-19 vaccination or a known ingredient within the COVID-19 in question, people who have a history of allergic reactions to vaccines or other sources can usually be safely vaccinated.[25]
[*] Pfizer-BioNTech is the name used for the Pfizer vaccine in the United States. The Moderna vaccine is in early stages of pre-approval, but is not currently available in Australia.
Non-severe, immediate allergic reactions are rare following COVID-19 vaccination.17 These reactions usually occur within a few hours and include hives, swelling, and wheezing (respiratory distress). These reactions usually resolve quickly without treatment. If a person has an immediate allergic reaction following their first COVID-19 vaccine, they should not have the second dose.
Severe allergic reactions (anaphylaxis) within minutes to hours are very rare following COVID-19 vaccines. The TGA found no evidence of increased risk of anaphylaxis associated with the AstraZeneca vaccine above the expected rate for any other vaccine.[26] Anaphylactic reactions to mRNA COVID-19 vaccines including the Pfizer vaccines is estimated to occur in only 2.5 to 11.1 cases per 1 million doses (0.025 % of people, or 2.47 per 10,000 individuals), and largely among people with known allergy history.[27]
Thrombosis and thrombocytopenia/TTS
Around the world and in Australia, very rare occurrences of blood clots with low platelet counts (thrombosis with thrombocytopenia/ TTS) have been reported following Oxford/AstraZeneca administration.[28],[29],[30],[31],[32] In Australia, there have been 37 confirmed, 23 probable cases, and two fatal cases of TTS following over 2.5 million doses given.[33] Although estimates of risk based on small numbers of cases are imprecise, the risk of TTS is estimated in Australia at around 3.1 per 100,000 in those <50 years and 1.8 per 100,000 in those ≥50 years.33
Conclusion
Both COVID-19 vaccines in Australia are effective and safe for the vast majority of recipients and also offer similar levels of protection against the new Delta variant. For most people, the benefits of receiving the COVID-19 vaccines outweigh the very remote chance of experiencing an adverse reaction. As the Australian COVID-19 vaccine rollout continues, it is important that nurses, midwives, and personal care workers get vaccinated if they can.
References
[*] Pfizer-BioNTech is the name used for the Pfizer vaccine in the United States. The Moderna vaccine is in early stages of pre-approval, but is not currently available in Australia.
[1] Pfizer. 2021. Pfizer and BioNTech Announce Vaccine Candidate Against COVID-19 Achieved Success in First Interim Analysis from Phase 3 Study [Online]. Feb 9 2021. Available: https://www.pfizer.com/news/press-release/press-release-detail/pfizer-and-biontech-announce-vaccine-candidate-against (Accessed June 30 2021).
[2] Voysey M, Clemens SAC, Madhi SA, et al. 2021. Safety and efficacy of the ChAdOx1 nCoV-19 vaccine (AZD1222) against SARS-CoV-2: an interim analysis of four randomised controlled trials in Brazil, South Africa, and the UK. The Lancet 2021; 397(10269): 99-111.
[3] Australian Therapeutic Goods Administration (TGA). 2021. COVID-19 vaccines [Online]. 2021. https://www.tga.gov.au/covid-19-vaccines (Accessed 30 June 2021).
[4] Australian Government Department of Health. 2021. Australian COVID-19 Vaccination Policy 2020 [Online]. Australian Government Department of Health. Available: https://www.health.gov.au/resources/publications/australian-covid-19-vaccination-policy (Accessed 30 June 2021).
[5] Ramasamy MN, Minassian AM, Ewer KJ, et al. 2020. Safety and immunogenicity of ChAdOx1 nCoV-19 vaccine administered in a prime-boost regimen in young and old adults (COV002): a single-blind, randomised, controlled, phase 2/3 trial. The Lancet 2020; 396(10267): 1979-93.
[6] Voysey M, Costa Clemens SA, Madhi SA, et al. 2021. Single-dose administration and the influence of the timing of the booster dose on immunogenicity and efficacy of ChAdOx1 nCoV-19 (AZD1222) vaccine: a pooled analysis of four randomised trials. The Lancet. 2021; 397(10277):881-91.
[7] ClinicalTrials.gov. 2021. A Phase III Randomized, Double-blind, Placebo-controlled Multicenter Study in Adults to Determine the Safety, Efficacy, and Immunogenicity of AZD1222, a Non-replicating ChAdOx1 Vector Vaccine, for the Prevention of COVID-19 [Online]. Available: https://clinicaltrials.gov/ct2/show/NCT04516746?term=NCT04516746&draw=2&rank=1 (Accessed 30 June 2021).
[8] Lopez Bernal J, Andrews N, Gower C, et al. 2021. Effectiveness of the Pfizer-BioNTech and Oxford-AstraZeneca vaccines on covid-19 related symptoms, hospital admissions, and mortality in older adults in England: test negative case-control study. BMJ. 2021; 373: n1088.
[9] Polack FP, Thomas SJ, Kitchin N, et al. 2020. Safety and Efficacy of the BNT162b2 mRNA Covid-19 Vaccine. New England Journal of Medicine 2020; 383(27): 2603-15.
[10] Dagan N, Barda N, Kepten E, et al. 2021. BNT162b2 mRNA Covid-19 Vaccine in a Nationwide Mass Vaccination Setting. New England Journal of Medicine 2021; 384(15): 1412-23.
[11] Menni C, Klaser K, May A, et al. 2021. Vaccine side-effects and SARS-CoV-2 infection after vaccination in users of the COVID Symptom Study app in the UK: a prospective observational study. The Lancet Infectious Diseases. 21(7):939-49.
[12] Hunter PR, Brainard J. 2021. Estimating the effectiveness of the Pfizer COVID-19 BNT162b2 vaccine after a single dose. A reanalysis of a study of ‘real-world’ vaccination outcomes from Israel. medRxiv 2021: 2021.02.01.21250957.
[13] Tenforde M, Olson S, Self W, al. 2021. Effectiveness of Pfizer-BioNTech and Moderna Vaccines Against COVID-19 Among Hospitalized Adults Aged ≥65 Years — United States, January–March 2021. MMWR Morb Mortal Wkly Rep 2021; 28 April.
[14] Mahase E. 2021. Delta variant: What is happening with transmission, hospital admissions, and restrictions? BMJ. 373:n1513 doi:10.1136/bmj.n1513.
[15] Public Health England. 2021. Public Health England monitoring of the effectiveness of covid-19 vaccination – 26 May 2021 [Online]. London: United Kingdom Government. Available: https://www.gov.uk/government/publications/phe-monitoring-of-the-effectiveness-of-covid-19-vaccination. (Accessed 30 June 2021).
[16] Bernal JL et al. 2021. Effectiveness of COVID-19 vaccines against the B.1.617.2 variant [Pre-Print Online]. MedRxiv. 2021.05.22.21257658. Available: https://doi.org/10.1101/2021.05.22.21257658 (Accessed 30 June 2021).
[17] Stowe et al. 2021. Effectiveness of COVID-19 vaccines against hospital admission with the Delta (B.1.617.2) variant [Online]. London: Public Health England. Available: https://khub.net/web/phe-national/public-library/-/document_library/v2WsRK3ZlEig/view_file/479607329?_com_liferay_document_library_web_portlet_DLPortlet_INSTANCE_v2WsRK3ZlEig_redirect=https://khub.net:443/web/phe-national/public-library/-/document_library/v2WsRK3ZlEig/view/479607266 (Accessed 30 June 2021).
[18] Centers for Disease Control and Prevention (CDC). 2021. What to Expect after Getting a COVID-19 Vaccine – June 24 2021. Online: https://www.cdc.gov/coronavirus/2019-ncov/vaccines/expect/after.html (Accessed June 30 2021).
[19] Hervé C, Laupèze B, Del Giudice G, Didierlaurent AM, Tavares Da Silva F. 2021. The how’s and what’s of vaccine reactogenicity. NPJ Vaccines 2019; 4(1): 39.
[20] Shimabukuro T. 2021. COVID-19 vaccine safety update – Jaunary 27 2021 [Online]. National Center for Immunization & Respiratory Diseases. Available: https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-01/06-COVID-Shimabukuro.pdf (Accessed 30 June 2021)
[21] Centers for Disease Control and Prevention (CDC). 2021. COVID-19 Vaccines and Allergic Reactions – March 4 2021 [Online]. Available: https://www.cdc.gov/coronavirus/2019-ncov/vaccines/safety/allergic-reaction.html (Accessed June 30 2021).
[22] Centers for Disease Control and Prevention (CDC). 2021. What to Do if You Have an Allergic Reaction After Getting A COVID-19 Vaccine – March 4 2021 [Online]. Avaialble: https://www.cdc.gov/coronavirus/2019-ncov/vaccines/safety/allergic-reaction.html (Accessed June 30 2021)
[23] Australian Therapeutic Goods Administration (TGA). 2021. AUSTRALIAN PRODUCT INFORMATION – COMIRNATY™ (BNT162b2 [mRNA]) COVID-19 VACCINE. 2021. Available. https://www.tga.gov.au/covid-19-vaccine-pfizer-australia-comirnaty-bnt162b2-mrna (Accessed June 30 2021).
[24] Australian Therapeutic Goods Administration (TGA). AUSTRALIAN PRODUCT INFORMATION COVID-19 Vaccine AstraZeneca (ChAdOx1-S) solution for injection. 2021. Avaialble: https://www.tga.gov.au/sites/default/files/auspar-chadox1-s-covid-19-vaccine-astrazeneca-210215-pi.pdf (Accessed Jun 30 2021).
[25] Glover RE, Urquhart R, Lukawska J, Blumenthal KG. 2021. Vaccinating against covid-19 in people who report allergies. BMJ 2021; 372: n120.
[26] Australian Therapeutic Goods Administration (TGA). 2021. AstraZeneca ChAdOx1-S COVID-19 vaccine: Update – Expert review finds no evidence of increased risk of anaphylaxis. 2021. https://www.tga.gov.au/alert/astrazeneca-chadox1-s-covid-19-vaccine-0 (Accessed 30 June 2021).
[27] Blumenthal KG, Robinson LB, Camargo CA, Jr., et al. Acute Allergic Reactions to mRNA COVID-19 Vaccines. JAMA 2021; 325(15): 1562-5.
[28] Greinacher A, Thiele T, Warkentin TE, Weisser K, Kyrle PA, Eichinger S. Thrombotic Thrombocytopenia after ChAdOx1 nCov-19 Vaccination. New England Journal of Medicine 2021.
[29] Schultz NH, Sørvoll IH, Michelsen AE, et al. 2021. Thrombosis and Thrombocytopenia after ChAdOx1 nCoV-19 Vaccination. New England Journal of Medicine 2021;384:2092-2101
[30] Cines DB, Bussel JB. 2021. SARS-CoV-2 Vaccine–Induced Immune Thrombotic Thrombocytopenia. New England Journal of Medicine 2021;384:2254-2256
[31] Østergaard SD, Schmidt M, Horváth-Puhó E, Thomsen RW, Sørensen HT. 2021. Thromboembolism and the Oxford–AstraZeneca COVID-19 vaccine: side-effect or coincidence? The Lancet 2021; 397(10283): 1441-3.
[32] Scully M, Singh D, Lown R, et al. 2021. Pathologic Antibodies to Platelet Factor 4 after ChAdOx1 nCoV-19 Vaccination. New England Journal of Medicine 2021;384:2202-2211
[33] Australian Technical Advisory Group on Immunisation (ATAGI). 2021. ATAGI update following weekly COVID-19 meeting – 9 June 2021 [Online]. Australian Government Department of Health. Available: https://www.health.gov.au/news/atagi-update-following-weekly-covid-19-meeting-9-june-2021 (Accessed 30 June 2021).
Author
Micah DJ Peters PhD works at the the National Policy Research Unit (Federal Office), Australian Nursing and Midwifery Federation (ANMF) and the University of South Australia, Clinical and Health Sciences, Rosemary Bryant AO Research Centre