Flashing a reassuring smile. Giving the thumbs up. Offering a comforting hand. A subtle, yet often powerful tool, the importance of body language has long-been recognised in nursing for its ability to improve patient care.
Anita Haines is a clinical nurse consultant at Western Health in Victoria and team leader of its Palliative Care Consultancy Service, which provides palliative care expertise and advice across the health service’s acute public hospitals.
Anita, who trained as a nurse in the UK, learnt about the importance of body language during the early stages of her career. Starting out, advice tended to centre on professional appearance and demeanour, for example, no hands on hips or folding arms, no slouching and standing up straight.
Throughout her career, Anita has witnessed both good and poor examples of body language.
One incident springs to mind, where a doctor stood nonchalantly in a doorway, with his hand leaning against the door frame, before breaking bad news to a family and walking off. His poor body language left the family angry and distressed.
While working in palliative care over the past 14 years, Anita says shaking hands with family members and patients has been one form of body language she uses to build a rapport. Other examples include using hand gestures to determine pain levels and sitting down and leaning in when talking to patients, which she believes conveys engagement, interest and approachability.

“I think it’s another way of demonstrating our compassion and our care,” she says of body language.
“One of the gestures I use a lot, that I wasn’t really aware of, was I’ll often put my hand over my heart when I talk to the patient or the family. It’s just me trying to reassure them that we will do the best for their relative or our best to make sure that they don’t suffer and are pain free and comfortable. I have that hand to the heart just to try and express my genuineness, my concern and compassion.”
In the wake of the COVID-19 pandemic, body language as a nursing tool has arguably never been more important.
In many ways, the pandemic has changed the way nurses deliver care. The new normal includes personal protective equipment (PPE) including masks, goggles and face shields and restricted interactions with patients where necessary.
Like many health services across the globe, the COVID-19 pandemic triggered a number of challenges for clinical nurse consultants (CNCs) at Western Health’s Palliative Care Consultancy Service.
Maintaining the service during the peak of the pandemic in Victoria, while donning restrictive, but necessary, PPE, without doubt created a barrier between patients, families and staff.
For example, wearing PPE made it difficult to hear and communicate with patients.
CNCs at the service are experts in preparing families for dying and face-to-face bereavement support. During COVID-19, nurses found it confronting being repeatedly exposed to a new level of loneliness and distress among patients.
The CNCs say many patients had no visitors and that they felt restricted by PPE because patients could not see their facial expressions or a comforting smile.
During this challenging time, Anita suggests direct eye contact and head movement became important tools in conveying reassurance and comfort to patients.
“I think our eyes really became our big way of communicating, where culturally appropriate.”

With body language, it is important to keep things positive. While looking at someone directly in the eye can express confidence and trust, unwavering eye contact can have the opposite effect, and come across as scary and offensive among some cultures.
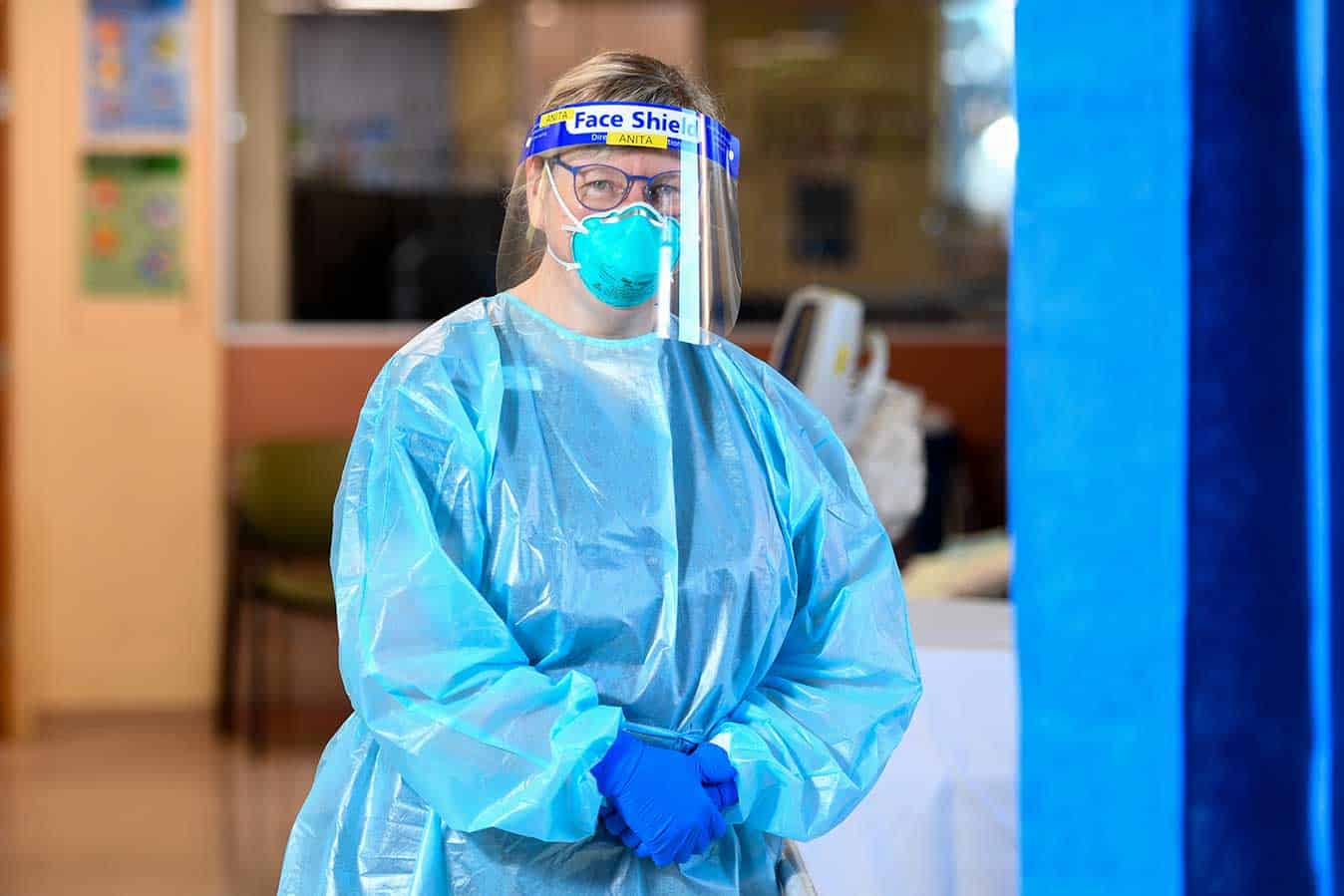
To hone her body language in a bid to improve care for patients, Anita took to practising smiling in the mirror with a mask on to see what expression her eyes, and even eyebrows, conveyed. She also printed her name across the front of her face shield so that patients felt more at ease.
Western Health is currently COVID-19 free and has returned to relative normality. Masks and face shields are still mandatory in many areas, which means using body language as a tool will remain important.
For nurses looking to improve their body language, Anita’s advice is practice makes perfect.
“Go home and put your mask on and practice in the bathroom. It’s certainly one of the things I remember doing early on,” she says.
“What do I look like? How do I express that genuine compassion that I feel? How do I express my care for patients? How do I show that through my eyes?”