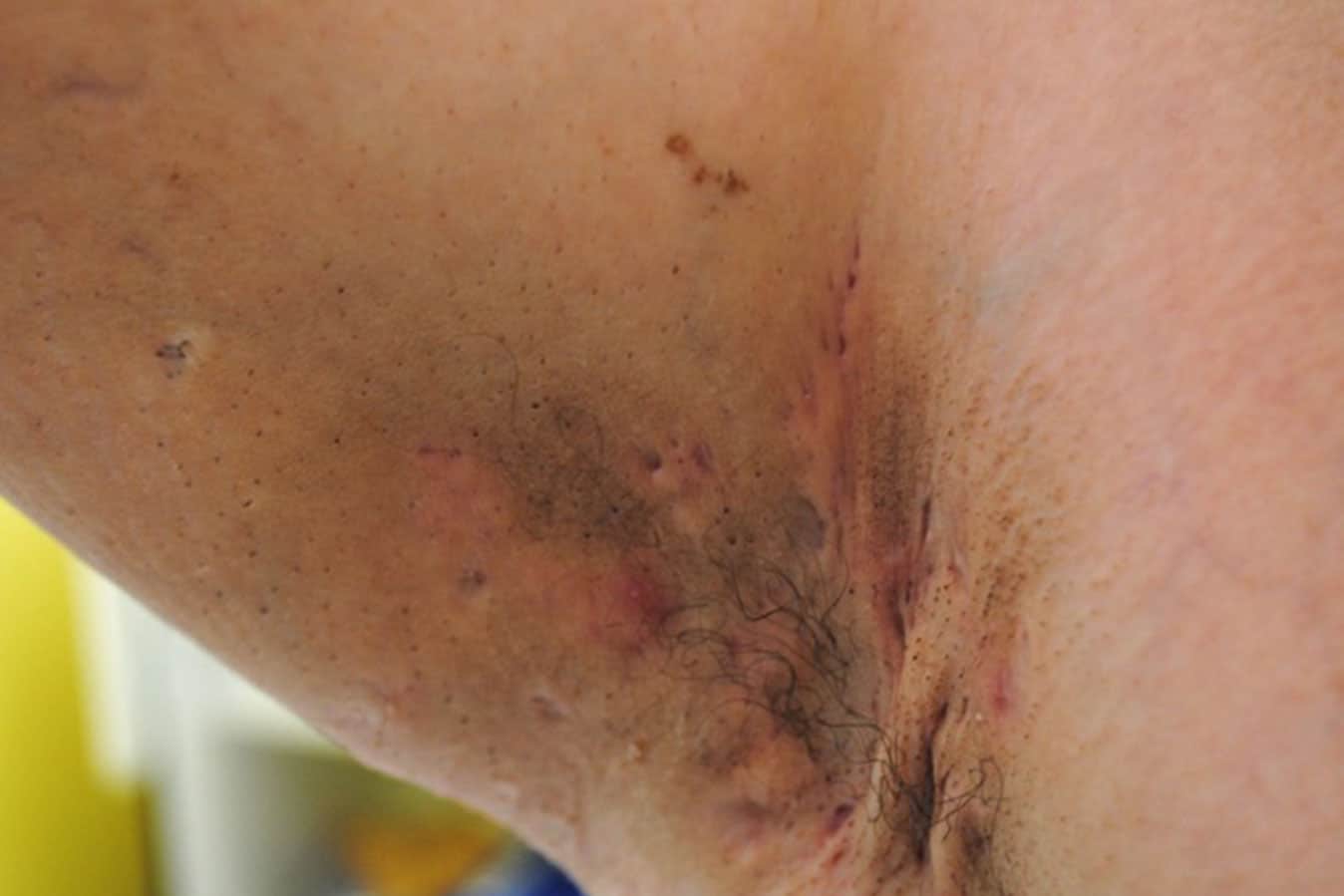
Hidradenitis suppurativa (HS) is a chronic autoinflammatory skin condition characterised by recurrent deep and painful nodules and abscesses (Vekic et al. 2018).
These lesions are predominantly located in the skin folds, such as the axillae, groin and intergluteal regions. It is also characterised by the presence of characteristic multi-headed comedomes, the development of sinus tracts and thick rope-like scarring (Jemec 2012).
Who gets HS?
HS most commonly affects individuals between 20 and 50 years of age, but there are cases of it occurring in prepubescent children.
Women are more frequently affected than men, with a ratio of 3:1 (Jemec 2012; Vekic et al. 2018).
One study demonstrated a prevalence of 0.67% in Australia (Calao et al. 2018). However, a point prevalence of up to 4% has been reported in the literature (Jemec et al. 1996).
It is likely that patients and their doctors may not recognise the disease, and therefore the prevalence in Australia may be higher (Vekic et al. 2018).
HS is associated with the lowest quality of life of all dermatological diseases. It frequently causes sufferers significant physical pain, psychological distress and impaired functioning.
Patients with HS may feel embarrassed by the appearance and odour of the lesions, and experience stigma from others due to lack of knowledge and understanding of the disease (Vekic and Cains 2017).
Patients with HS may also need to take additional sick leave to manage their condition or require alternative duties, which in turn may impact upon their employment opportunities, career progression and financial stability.
How is it diagnosed?
Diagnosis is made based on clinical examination and history.
It is a diagnosis of exclusion, meaning that it is important to rule out more common conditions prior to making a diagnosis. There are no diagnostic laboratory or imaging tests.
It often takes several years for patients to receive a diagnosis, with reports of average times to diagnosis from five to 12 years from disease onset (Jemec and Kimball 2015; Harrison et al. 1991; Mebazaa et al. 2009; Saunte et al. 2015). It is commonly mistaken for skin infection, such as boils.
What diseases is HS associated with?
HS is associated with a number of co-morbidities and lifestyle factors including metabolic syndrome (insulin resistance, type II diabetes, hyperlipidaemia, polycystic ovarian syndrome and obesity), pilonidal sinus, depression and tobacco smoking (Vekic et al. 2018).
Both obesity and tobacco smoking are associated with worse disease compared to non-obese and non-smoker HS patients (Sartorius et al. 2009).
How is HS managed?
Medical management of HS is dependent upon disease severity.
Mild to moderate disease is frequently managed with topical or oral antibiotics (Vekic and Cains 2018).
Patients with moderate to severe HS may qualify for adalimumab, an anti-TNFa via the Pharmaceutical Benefits Scheme.
Approximately 40-60% of patients respond to this treatment, with response being defined as a reduction at 12 weeks from baseline in abscess and inflammatory nodule count by 50% (Kimball et al. 2016).
Surgery may be indicated in some patients with large and or persistent lesions not responsive to treatment.
Surgical treatments used in HS include incision and drainage, deroofing and excision with or without grafting of affected areas (Vekic and Cains 2018).
Actively discharging lesions should be dressed with a non-adhesive absorbent dressing.
The anatomical location of these lesions can make dressings difficult, and dressings will often require taping down.
The aim of dressings is to minimise pain, odour and friction (Vekic and Cains 2017).
Patients with HS often benefit from low impact exercise and weight loss through improvement to their insulin resistance.
What should I do if I think a patient has HS?
Nursing staff may be the first healthcare workers to identify cases of HS, as they perform skin examination during showering and during Waterlow assessments. Patients may also complain of skin issues directly to nursing staff.
If you suspect a patient has HS, first clarify with them if they have been diagnosed with this condition.
If they have not been diagnosed, and the patient is in hospital, you should discuss it with the patient’s treating team and raise your concerns that the patient may have HS.
If instead the patient is seen in the community, you should instead liaise with their GP.
All patients with suspected hidradenitis suppurativa should be referred to a dermatologist for formal diagnosis and management.
Patients with HS can be referred to an Australian Facebook-based support group called “HS Sufferers in Australia” (https://www.facebook.com/groups/hssufferersinaustralia/).









One Response
HS is a relatively common and extremely burdensome inflammatory skin condition that is not well-recognised other than the dermatologist; yet, the clinical presentation is distinct and awareness of common risk factors, possible comorbid conditions and patient-reported quality of life can enable a reliable diagnosis. It occurs most frequently in post-pubescent women, and sex differences have been identified. Risk factors for HS include smoking and obesity, which may also be associated with more severe disease. About one-third of patients report a family history of HS. HS has been reported to co-occur with several comorbid conditions—most notably, inflammatory bowel disease.