It was our ‘Ruby Anniversary’, 40 years since ‘Group 792’ from St Andrews Private Hospital, Adelaide, commenced our nursing training. We were a small group of 11, but eight of us had made it to our 2019 reunion in Canberra.
Half a lifetime ago, we were sheltered 17-year-old girls who together, over three years, learnt the formative, professional, and personal lessons of our young lives. Then, we mostly went our own ways. Now, 37 years later, as ‘middle-aged’ women, we reunited to share our life experiences. How would it go?
Six of the reunion group are still registered nurses (RNs):
Amanda works in palliative care, and Karena in recovery.
Sue(1) is a dermatology nurse.
Nicole is a midwife who has worked nights for the past 20 years, and Anne-Marie is a health informatics professional.
I am a PhD candidate undertaking research on the feasibility of nurse-led clinics for people with multimorbidity.
Only one of us is no longer nursing – Wendy is a tomato farmer.
All of us had enjoyed our many years in nursing. Nicole reflected:
“I get most of my rewards from the mothers I have helped in overcoming their initial fears with baby and breastfeeding, and have received lovely letters sent to me, months later, that has given me my greatest buzz”.
Sue recalled her time coordinating an IVF clinic:
“I spent the following month following up on all the women, enjoying the highs of those who were successful and providing a shoulder to cry on for those who were not. I loved every minute of it”.

It was universally agreed that now there is no such thing as an empty bed and that for nursing and midwifery high patient turnover is a common stressor.
As older nurses, we spoke about fast-paced workdays and the shifting perceptions of younger colleagues. Nicole observed:
“I feel that some staff resent the older person as we don’t practice the same way that they do and we are slow, and our priorities are often different. But, on the other hand, some younger nurses recognise our knowledge levels and respect us. I often question myself as to why the younger nurses seem to finish their rounds hours before me or do their feeds quicker. Are my time management skills lacking or do I just do more? I feel the latter but feel they don’t see it that way.”
Some of us felt occasionally ignored; our experience and knowledge overlooked and undervalued by younger staff. Others noticed they were sometimes sought out and valued because of their experience.
Nicole summed up the challenges we experience:
“Although the fundamentals of nursing have not changed, the pace at which we’re expected to deliver care, patient throughput and technology has escalated.”
Of course it wasn’t all serious! We relived past antics from our training and Amanda recalled the glamorous Matron, Miss Pitcher.
Big cheese in nursing administration, Miss Pitcher was a cross between sultry Lauren Bacall and innocent Sally Field as the ‘Flying Nun’. Standing six feet tall, with a slash of red lipstick, she cut a striking figure with her oversized aeronautical headwear!
I can’t really say ‘professional engagement’ with the student nurses was Matron Pitcher’s forte, but it certainly was for our clinical tutor Sister Voveris (or ‘Iced Vovo’ as we affectionately nicknamed her) who was a kindly, yet stern woman of Latvian heritage with a razor-sharp intellect lurking behind an imperious forehead. Wendy remembered that ‘Iced Vovo’ would find her skulking in ‘the backs’. Wendy would then be dragged out for random aseptic technique testing; was it up to scratch? Following the aseptic technique interrogation, she would be on a roll. Did the pillow cases open towards the windows? If not, on the spot bed re-making would be required. Were the commodes clean? Wheels and dressing trolleys thoroughly scrubbed? Were bins empty; jugs full; and bowel and pressure area books up to date? Were patients sitting upright and comfortable in bed- with their covers pristine- and all hygiene completed, by 10 am?
Then came the piece de resistance: Deputy Matron, Sister Le Poidevan (or ‘Le Poison’ as she was known). ‘Le Poison’ found me one Christmas morning, only to ask; “Nurse Bishop, have you ever seen a dead body”? My jaw dropped, clearly signaling that I hadn’t. I was then ushered respectfully into a room to lay out the body of an elderly gentleman with the good Sister. Why was she even working on Christmas morning?
Then, of course, we remembered the humiliations. Like the time third-year scout nurse Margaret was ‘playing’ with an elastic band whilst in theatre. Of course, she pinged it, dead centre, into the middle of the sterile field, mid-operation. The operating room team’s response? NOT HAPPY JAN, to put it mildly.
Margaret was relegated to tea duties for the doctors after that: “two for tea in theatre three” would be heard over the intercom, or was that “tea for three in theatre two”?
Nursing did have its positives though – like going on a ward round with Mr Plowczkieiczmi, that young, hot-blooded Hungarian hunk (also known as Mr. ‘please kiss me’).
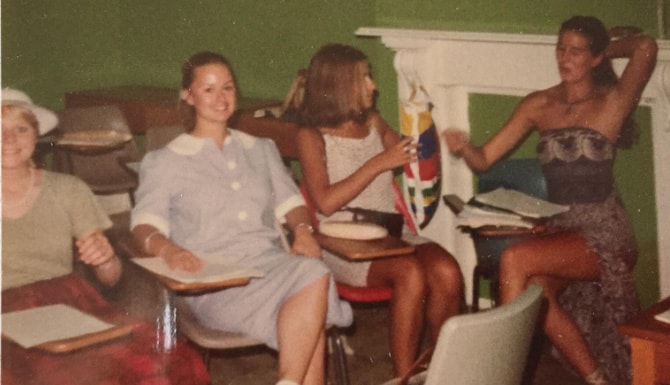
Looking back, we were nothing if not young and naïve, intimidated into politeness on those early ward rounds. The heady thrill of ‘charging’ the ward in our third years, along with the joy of passing each procedure test and slowly inching towards our collective dream of becoming Registered Nurses. We experienced appreciation and chocolates from patients and their grateful families, mixed with bullying and terror from the ward sisters. Despite this and our youthful inexperience, a gradual building of competence was evident.
Of course, those of us who didn’t continue with nursing have had full and interesting journeys. Ann says:
“I found my experience in nursing has helped in some respects with farming life, I have helped our sheep with births, wound healing, and general first aid on the farm”.
Ann is glad that she nursed so many years ago, but wouldn’t return to it. Wendy talked about her life on a Northern NSW farm, where she reluctantly gave up nursing when it became too difficult to manage the farm, sell organic produce locally and raise six children. More recently, she has faced extreme drought and devastating bush fires, an experience resonating throughout Australia.
On a personal level, we have all been through the ups and downs of life; confronted with the death of partners and, devastatingly, children.
We had weathered separation and divorce, children’s mental and physical health issues, children longed for and never born, as well as the joys of our own, partners, children’s and even grandchildren’s achievements.
Despite our disparate personal and professional experiences, we rediscovered a shared love of nursing and enduring close bonds based on our earlier formative experiences together. We still love to care for people; to make them comfortable; relieve their pain and most of all, provide them with dignity.
Despite being challenged with a progressively complex health system we continue to find satisfaction in educating and empowering our patients.

Our 40 year anniversary, much like the ruby that represents the passing of this significant period of time, celebrates these nurses, educated in a very different era and way; and how they brought passion and commitment for nursing into their patients’ lives. Given the ruby’s hue is so close to the colour of blood, which carries life-giving oxygen, the gemstone, much like these nurses, is also said to represent vitality and vigour. In their own unique way this group of skilled and caring practitioners, even after 40 years, remain an integral part of the professional cornerstone of the health workforce.








One Response
Thank you for your article; my group will be celebrating our 35 years since graduation this year (2020) and we are in the process of trying to find everyone. We were one of the last groups to train in the hospital system at Hornsby Hospital.
I am disheartened at the level of nursing care in our wards today. From personal experience, I can honestly say that nurses do not ‘nurse’ any more and this is why they finish their rounds so quickly (as you stated above). Their nurse to patient ratio is a lighter load than it used to be yet they still believe that they are overworked. In a 7 day stay in a public hospital a couple of years ago (major surgery), not one nurse came into my room to ask me; how I was feeling, to ask if I needed any help or to check that I could reach my food or water. It was so upsetting to see how the professional standards had deteriorated. There is still the odd nurse that may show some empathy but they are few and far between.